Referral Pathways
Recognizing the early warning signs is the first vital step toward a cure; taking immediate action is the next. To ensure your child receives the best possible care, it is critical to follow the established referral pathways. These protocols are designed to move your 'Young Warrior' quickly from a local clinic to the specialized oncology experts they need to begin their journey to recovery without delay.
After a young person with suspected cancer has been identified, the next step is to follow the correct referral pathways for the nearest paediatric oncology unit (POU) where multidisciplinary, comprehensive care across specialties can be offered. This is to enable children to reach the specialised treatment centres in time to ensure effective treatment, as well as have access to essential medicine and care.
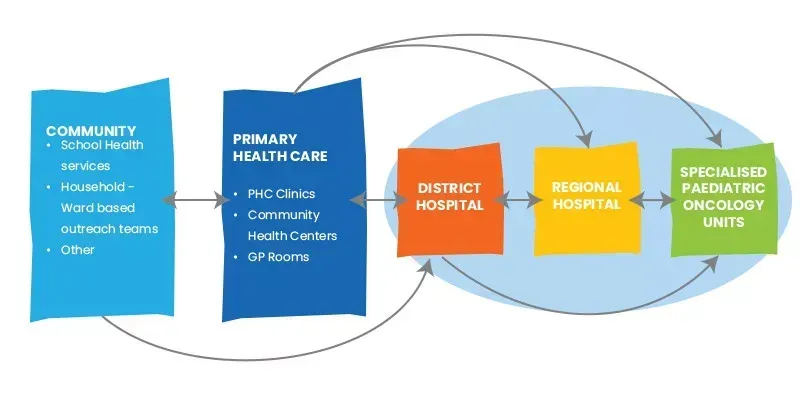
The pathway from the first point of entry at Primary Health Care level to specialised POUs is theoretically a clear and uncomplicated one.
For most young people who have a possible diagnosis of cancer, the point of entry into the health system is through primary health care (PHC) services either at the local PHC Clinic, Community Health Centre, local General Practitioner (GP) and/or traditional healer.
At CCO, we advocate for emphasis to be placed on increasing capacity in community-based and primary health services to facilitate prompt referral to specialist centres without having to go through convoluted pathways. Provincial Referral Policies should outline clear referral pathways for patients with a cancer diagnosis and institutions should have local standard operating procedures (SOPs) with contact details of the nearest POUs to ensure appropriate, timely and reliable transport of the patient to the treatment facility after liaising with the POU and after stabilising the patient.
The centres will have the necessary human resources available namely; paediatric oncologists, paediatric oncology-trained nursing staff, radiation oncologists, surgeons, histopathologists, radiologists, supportive care and intensive care unit facilities. Laboratory facilities for the processing of biopsy material for morphological diagnosis as well as cytogenetic and molecular analysis of the tumour tissue are required. Limited availability for these tests is currently available within the National Health Laboratory Service (NHLS) attached to large tertiary facilities. It is imperative that the young patient with suspected cancer be referred for imaging and diagnostic investigations to be done at the referral centre to avoid delay in referral and to ensure that the appropriate investigations are performed, thus preventing further delay and waste of money.
What do I need to bring with me?
A referral letter from the doctor who is currently treating the child
All the tests that have been done before – especially the dates when the tests have been done
The slides of any previous bone marrows that have been done
All of the child’s documentation/files that can support the case is needed
For a list of Paediatric Oncology Units in South Africa, visit:
https://www.saccsg.co.za/About/Centres
1. What is childhood cancer, and how is it different from adult cancer?
Childhood cancer is a disease of the body’s cells that develops in growing tissues like blood, bone marrow, and kidneys. Unlike adult cancers, childhood cancer is not lifestyle-related (it is not caused by smoking, diet, or environment) and often responds much better to treatment because children’s bodies have a higher capacity for healing.
2. Is childhood cancer curable?
Yes. With early detection and specialized medical care, 70–85% of childhood cancers are curable. Our mission at CCO is to bridge the gap between diagnosis and survival so that every "Young Warrior" in Lesotho has the chance to thrive.
3. What are the "St. Siluan" Early Warning Signs?
The St. Siluan signs are a life-saving checklist to help you spot potential symptoms. They include:
S – Seek medical help for persistent symptoms.
I – Eye changes (white spots or new squints).
L – Lumps or unexplained swellings.
U – Unexplained fever, weight loss, or bruising.
A – Aching bones or joints.
N – Neurological signs (changes in balance or speech).
4. Is childhood cancer contagious?
No. Childhood cancer is not a "catchable" disease. It is safe and encouraged to hug, play with, and support children undergoing treatment. It is also not caused by "bad luck" or "punishment"—it is a biological medical condition.
5. Does CCO provide medical treatment?
CCO does not provide medical treatment directly. Instead, we work through a formal MOU with the Ministry of Health to support the child’s medical journey. We focus on holistic care, providing the logistical, emotional, and financial support families need to access specialized oncology services.
6. How does CCO support families traveling for treatment?
Many children in Lesotho require specialized care at centers in Bloemfontein, South Africa. CCO provides essential transport and lunch packages for these trips to ensure that no child misses a life-saving appointment due to financial barriers.
7. Who is eligible for support from CCO?
We support children under the age of 16 in Lesotho who have been diagnosed with cancer or life-threatening blood disorders. Currently, we are walking the journey with 53 brave children and their families.
8. How can I refer a child to CCO?
If a child shows persistent warning signs, they should first visit their local clinic or doctor. Once a potential case is identified, the medical team will follow the referral pathway to specialized care. Parents or health workers can contact CCO directly to begin receiving logistical and emotional support during this transition.
9. Why is early detection so important?
Early detection is the single most important factor in survival. When cancer is caught in its early stages, it is less likely to have spread, making treatment more effective and less invasive. Our outreach campaigns aim to move children from "late-stage" diagnosis to "early-stage" healing.
10. How can I help Lesotho’s Young Warriors?
There are three main ways to join our mission:
Donate: Funds go directly to transport, nutritious meals, and emotional care.
Partner: We welcome corporate and institutional collaborations.
Volunteer: Share your professional skills or your voice to spread awareness in your community.
"Bringing hope, one child at a time".

At CCO, we are committed to nurturing the hope and well-being of Lesotho’s Young Warriors. We are honored to be a part of their path to recovery. Stay connected with us for vital early detection tips, survivor stories, and updates on how we are bringing hope, one child at a time.

Quick Links
Resources
Connect With Us
© CCO. 2026. All Rights Reserved.